Harbor TMS Therapy Center
Transcranial Magnetic Stimulation
Transcranial magnetic stimulation (TMS)—also called repetitive transcranial magnetic stimulation (rTMS) — is a noninvasive technique used in the treatment of a variety of mental health conditions, such as migraine pain, obsessive-compulsive disorder, and especially, depression. TMS is typically prescribed when antidepressants have failed, or the side effects are intolerable. TMS Therapy is:
- Safe & effective; minimal side effects
- Non-invasive
- No Anesthesia; outpatient treatment
- Accepted by most insurance providers, including Medicare
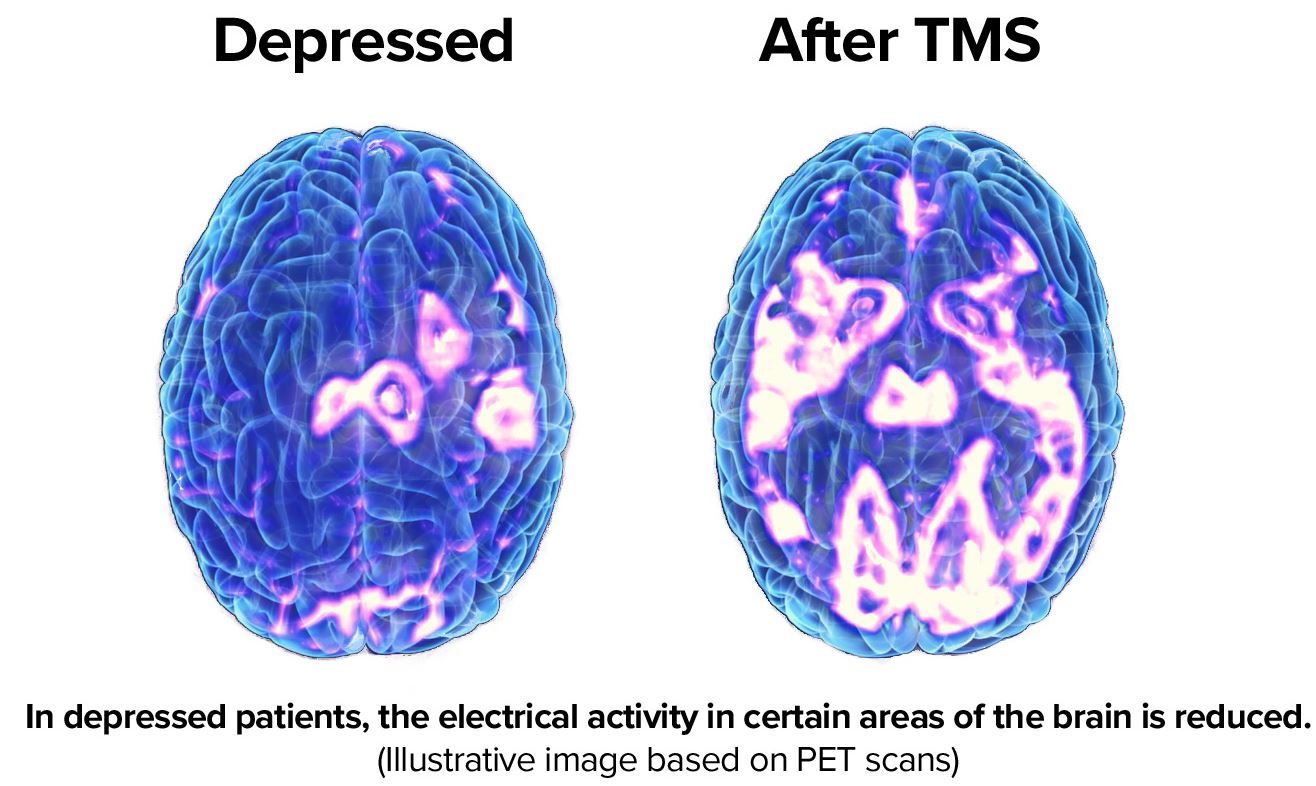
What is TMS Therapy?
TMS Therapy involves a series of repetitive, brief, and highly focused magnetic pulses, designed to stimulate brain cells. TMS is typically prescribed to adult patients when antidepressants have failed, or the side effects are intolerable. In comparison to antidepressants, TMS Therapy is a non-invasive outpatient procedure with few known side effects. Transcranial magnetic stimulation delivers short magnetic pulses to specific regions of the brain. It does so to stimulate the neurons in those areas. TMS is non-invasive and requires no anesthesia. Therefore, during the session, the patient remains awake and alert.
What happens in a TMS session?
Because the treatment involves magnets, patients are first asked to remove metallic items (e.g., jewelry). They are also provided with earplugs because the TMS machine produces loud clicking sounds while delivering pulses. The patient then sits comfortably in a chair while the technician determines the intensity of stimulation needed by delivering a few brief pulses and checking the patient’s motor reaction.
Subsequently, the stimulation coil is placed next to the target area, which is usually the prefrontal cortex (the front part of the brain). Then the device begins delivering pulses. These pulses cause brief activity in the brain cells in the target area. The length of the session depends on numerous factors (e.g., the coil, the protocol), but it is usually less than an hour. The treatment is typically repeated five times a week, for about four to six weeks. Since anesthesia is not used during the treatment, once the session is over, the patient can get back to normal life right away. Compared to common medical treatments for depression, like antidepressants, TMS has fewer side effects. Perhaps the most common side effect of TMS is a headache. TMS is a safe and well-tolerated treatment that is not associated with any of the systemic side effects typically experienced with antidepressants. Clinical studies show that the most common side effects are mild to moderate scalp discomfort and mild headaches, both of which are short-term.
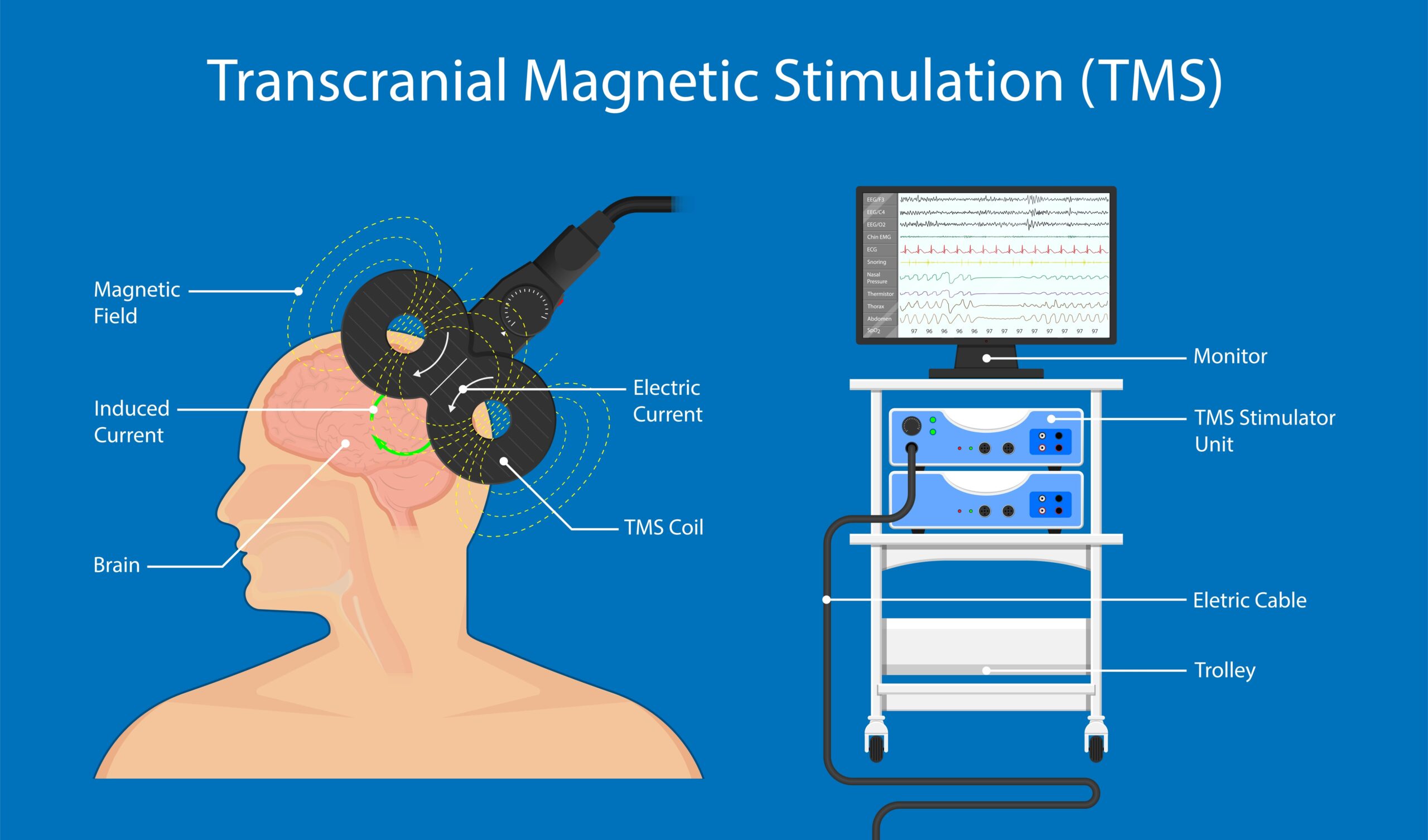
TMS for treatment of depression disorder
According to the Diagnostic and Statistical Manual of Mental Disorders (DSM–5), major depressive disorder is characterized by depressed mood, reduced feelings of pleasure, weight loss or weight gain, sleeping too much or too little, motor changes (e.g., agitation), fatigue, feelings of worthlessness, concentration difficulties, and thoughts of suicide. Sometimes psychotherapy and medications work well for depression. Some patients, however, who do not find relief, have found new treatments like TMS helpful.
TMS has received considerable research attention for treating a variety of mental health conditions, especially depression. For instance, a randomized clinical trial, funded by the National Institute of Mental Health, found that three times as many people receiving TMS, compared to a sham treatment, experienced remission of depressive symptoms. Note, sham treatments are used to rule out psychological and various other factors that may explain the positive results of a study. In short, the use of sham treatments increases researchers’ confidence in their findings.
A related question that has less of a clear answer is the question of how TMS improves depression. The exact mechanisms are not known but are probably related to how electromagnetic induction changes the excitability of neurons in brain areas related to depression. Note, high-frequency stimulation (e.g., ≥ 5 Hz) is used to increase neuronal excitability, while low-frequency stimulation (≤ 1 Hz) is used to decrease neuronal excitability. In the treatment of depression, the targeted area is often the dorsolateral prefrontal cortex, which is involved in cognitive control and regulation of emotions. The goal of TMS therapy is to produce lasting, positive changes in the functioning of these areas.
Contact Us
Harbor TMS Clinic
4631 Teller, Suite 100 Newport Beach CA 92660
(949) 486-5991
tms@harbormentalhealth.com
Get in touch
Health Insurance
About us
Contact us
About Harbor Psychiatry & Mental Health
We believe outstanding healthcare is delivered when we merge the science of medicine with the compassion of our hearts. We refer to this as “head and heart together,” inspiring constant improvement and lasting success.
Psychiatrists Orange County CA
Psychologists Orange County CA
Contact us
Address: 4631 Teller, Suite 100
Newport Beach CA 92660
Phone: (949) 486-5991
Email: tms@harbormentalhealth.com
