What is Dual Diagnosis?
Dual Diagnosis is a term that is frequently used in the mental health and addiction recovery communities. Understanding what Dual Diagnosis means can be confusing since many drug and alcohol treatment programs describe themselves as being a “Dual Diagnosis program” even if they lack the specific expertise to effectively treat serious mental health issues.
Dual Diagnosis, also called Co-occurring disorders, describes the experience of having both an alcohol/drug or other addiction and a mental health disorder. Sometimes the addiction comes first, other times the mental health illness develops first. Frequently, a person with a serious mental health condition such as bipolar disorder, major depression, severe anxiety may use alcohol, drugs, or behaviors such as gambling, eating, and sex as a way to self-medicate their mental health symptoms.
Is Dual Diagnosis common?
Estimates of the number of Americans who have both an addiction and mental health illness range from 8 to 10 million. The 2018 National Institute on Drug Abuse (NIDA) reports that “about half of people who experience a mental illness will also experience a substance use disorder at some point in their lives and vice-versa.
Figure 1: Co-Occurring Substance Use Disorder and Serious Mental Illness in Past Year among Persons Aged 18 or Older
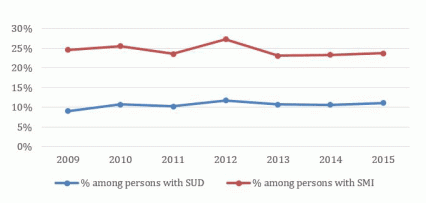
Source: SAMHSA, Center for Behavioral Health Statistics and Quality, National Survey on Drug Use and Health, Mental Health, Detailed Tables.Available
Which comes first: addiction or mental health illness?
While it is difficult to determine if addiction or mental health illness occurs first, most researchers and clinicians recognize that the presence of one will complicate the other. An addiction to a drug, alcohol or a behavior such as gambling or sex, may begin as a way of relieving feelings of sadness or worry or fear, but eventually worsens these feelings.
What are some of the mental health conditions that frequently occur along with an addiction?
In many cases, individuals with the following mental health condition also experience a drug, alcohol or other addiction:
Depression, anxiety, a mood disorder such as major depression or bipolar disorder, eating disorders such as anorexia, binge eating or bulimia, psychotic disorders such as schizophrenia or delusions, anxiety, and obsessive-compulsive disorders, PTSD, and personality disorders such as borderline or narcissistic disorder. Many individuals with chronic pain, fibromyalgia, cancer, diabetes, auto-immune diseases, brain injury, and HIV may develop both an addiction and a mental health disorder.
What is a Dual Diagnosis treatment program?
Before the 1980’s most treatment programs for addiction and mental health were separate. The general treatment approach required the individual to “get clean and sober” before beginning treatment for his or her mental health illness. In the 1980’s, treating dual diagnosis often consisted of adding a 12 Step program such as Alcoholics Anonymous to a mental health program. Although this was a positive first step, the results were not very good. Current research indicates that the best treatment for dual diagnosis integrates mental health and addiction provided by highly skilled medical and clinical behavioral health professionals. Since mental health illnesses are often severe and complex, special training and experience in the treatment of personality disorders, eating disorders, PTSD, long-term major depression, or severe anxiety is required. While 12 Step fellowship meetings and education groups can be helpful, these do not adequately address the seriousness of a dual diagnosis.
What are the specific challenges to treating Dual Diagnosis?
Treating a dual diagnosis requires an integration of medical/psychiatric and highly trained clinical professionals. Many individuals who have a dual diagnosis find themselves in a treatment program or residential treatment center that does not have the medical and clinical expertise to treat both. In order to recover fully, an individual who has a dual diagnosis is best treated in a program that offers psychiatric / medication options and specific psychotherapy interventions that are designed to treat serious mental health conditions. Treating serious mental illnesses such as bipolar disorder, severe anxiety, PTSD, major depression and personality disorders requires more than educational groups or group therapy.
How does Harbor Psychiatry and Mental Health treat Dual Diagnosis?
HPMH offers an integrated outpatient dual diagnosis treatment program. This means our psychiatric team and doctoral-level psychologists work closely to develop a treatment plan that integrates medication management, when needed, with specific psychotherapy interventions. HPMH’s psychologists possess expertise in identifying and providing the best approach to treat an individual’s dual diagnosis. Years of experience and doctoral level training underpin our skill at helping our clients recover from addiction and manage mental health illness.

